High blood pressure is of the conditions of metabolic syndrome. One-third of adults in the United States have metabolic syndrome increases the risk of heart disease, stroke, and type 2 diabetes. Intermittent fasting has become increasingly popular for managing blood pressure and other metabolic syndromes over the years. In this article, I will briefly talk about what is high blood pressure with its associated risk, and the smart steps to smartly manage blood pressure through intermittent fasting.
High Blood Pressure and Its Risks
High blood pressure or hypertension is one of the most common disorders worldwide. Nearly half of adults in the United States (47% or 116 million) have hypertension, which is defined as a systolic blood pressure >130mmHg, a diastolic blood pressure >80mmHg, or on any medication for hypertension(1).
Hypertension is a condition in which the force of blood against the artery wall is too high and extra workload is put on the heart. Therefore, it is a risk factor for cardiovascular disease, stroke, chronic kidney disease, and damage to blood vessels in the eye and kidney if left uncontrolled.
Intermittent Fasting and Blood Pressure
Intermittent fasting has been shown to associate with health benefits including a reduction in blood pressure. Numerous studies have demonstrated that alternate-day fasting with a 25% energy restriction (around 500-600 calories on fasting days) reduced blood pressure among overweight and obese individuals. Our body is complicated, thus the reason for such a result is therefore complex(2,3,4,5).
A study with a fasting program completed with a daily intake of only 250 calories suggested when following a fasting regimen, the subjects went through a reduction in sodium intake, daily stress cutting, hormone level changes for fluid balance, and the increased neurotransmitter which expands the blood vessels all contributed to the reduction of blood pressure. Long-term fasting tends to decrease blood pressure and the effect persisted after food reintroduction(6,7).
Although you may not practice your fasting at such an intense level, simply extending your fasting window to at least 16 hours a day can help you reduce your sodium intake from food, reduce stress level and other changes in your body could all contribute to blood pressure reduction.
Must-Read Tips to Start Intermittent Fasting with Hypertension
Choose a Suitable Fasting Plan: to Determine How Long You’ll Keep Fasting
Intermittent fasting can be done through different fasting plans based on different lifestyles and daily schedules.
Although studies demonstrated promising results were based on alternate-day fasting with significant calorie restrictions. However, a time restrictive fasting with a minimal 12-16 hours daily can still provide health benefits to reduce blood pressure and improve cardiovascular disease risk factors. Starting simple is still better than starting nothing.
To start fasting, it’s simple to choose a lower-level fasting plan such as 12:12 or 14:10. Stay at the lower-level plan for at least one to two weeks and monitor how you feel. If you haven’t experienced any discomfort and the plan seemed easy and manageable, you may increase the intensity by extending your fast plans to 16:8, 18:6, or even 20:4. Remember, try to get the best fasting plan since it’s the one you can do for the long term.
Plan Your Meals for Eating Window: to Select Your Diet
Now that your fasting plan has been determined, it’s time to select what you eat during your eating window. As you’re fasting, you are eating less food overall. Therefore, it is important to make smart food choices to maintain your necessary nutrients. Planning food types in your meals and reasonable portion sizes are essential elements to help to achieve your weight goal as well as manage your blood pressure. During your eating window, plan for two main meals and one to two snacks with healthy food for hypertension.
Follow DASH Diet
Although there is no food restriction following intermittent fasting. Diet still plays a key role in successful hypertension management. Dietary Approaches to Stop Hypertension or DASH is a diet designed for people with hypertension.
If you have started fasting and not following a specific diet now or have a diet that mainly contains processed foods and takeaways, I will highly recommend you to combine your fasting with the DASH diet which not only emphasizes healthy food sources to reduce salt/sodium intake, limits fat and added sugar for heart health but also reduce overall calories to assist weight loss.

Apart from reducing sodium, fat, and added sugar. DASH diet also encourages foods that are rich in potassium, magnesium, and calcium which all play an important role in helping your body to regulate blood pressure.
- Potassium source: banana, organs, apricots, melons, dry fruits, dark leafy greens, mushrooms, cucumbers, zucchini, pumpkins
- Magnesium source: nuts & seeds, beans, nut butter, breakfast cereals, dark chocolates, whole grains.
- Calcium source: dairy products, nut/plant-based milk fortified with calcium, breakfast cereals, almonds, sardines, canned tuna, seeds, dark leafy greens,
Reduce Sodium Level
In the process of following the DASH diet to optimize your quality of nutrition, reducing sodium intake is one of the main philosophies. Here are some simple swapping ideas to help you reduce your sodium intake(8).

Stay Active
Regular exercise is a good way to help you distract from fasting, manage stress as well as reduce blood pressure and risk of cardiovascular disease. No matter hypertension or not, fasting or not, regular exercise is always needed for everyone at any time.
The American College of Sports Medicine recommends individuals to engage in different types of exercise with progression over 4 to 6 weeks to achieve the volume of 150 minutes per week of moderate-intensity exercise as recommended by the hypertension management guideline(9).
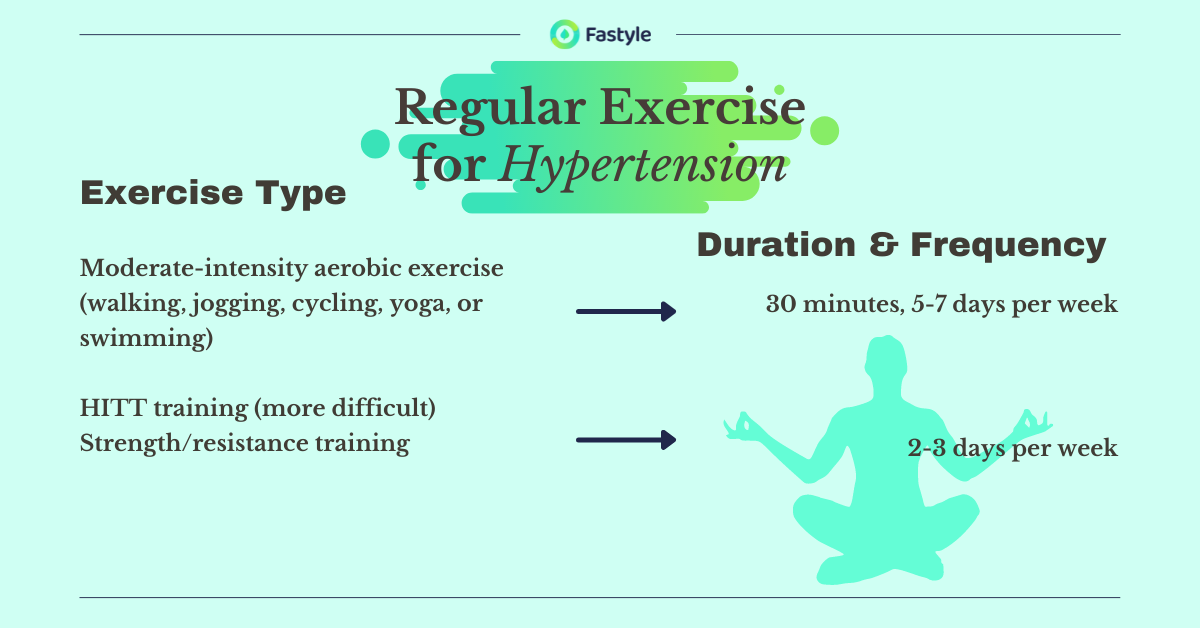
To put these recommendations into practice and begin a regular exercise, you may follow this example guide to structure your personal exercise plan. It is designed with slow progression to meet the target 30 minutes daily or 150 minutes per week moderate-intensity guideline.
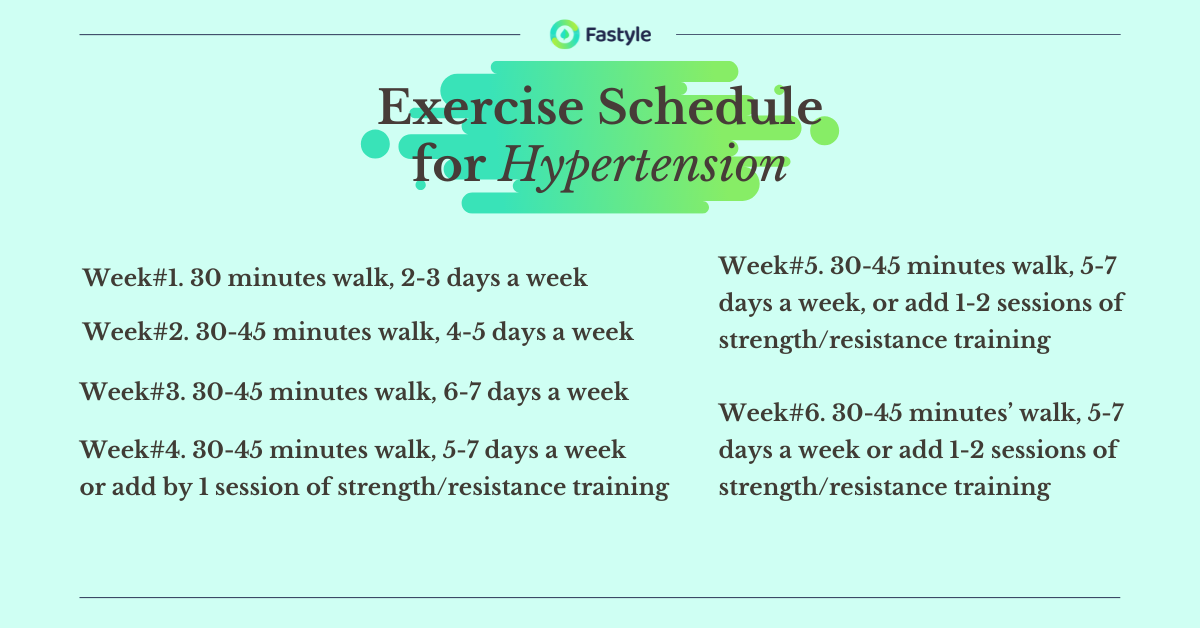

Summary:
- Hypertension is a major risk factor for cardiovascular disease and can be dangerous if let unmanaged.
- Intermittent fasting can reduce blood pressure and therefore lower cardiovascular disease and other health risks.
- Choose lower intensity fasting plan to start with and plan eating window following DASH diet and reduce sodium intake.
- Plan for regular exercise and increase intensity with slow progression to meet the target load recommended by hypertension management guideline.
Reference:
- https://www.cdc.gov/bloodpressure/facts.htm
- https://pubmed.ncbi.nlm.nih.gov/24215592/
- https://pubmed.ncbi.nlm.nih.gov/20921964/
- https://pubmed.ncbi.nlm.nih.gov/19793855/
- https://pubmed.ncbi.nlm.nih.gov/23497604/
- https://www.ahajournals.org/doi/10.1161/JAHA.120.018649
- https://pubmed.ncbi.nlm.nih.gov/30897855/
- https://www.health.qld.gov.au/__data/assets/pdf_file/0025/150577/renal_lowsalt.pdf
- https://www.acsm.org/blog-detail/acsm-certified-blog/2019/02/27/exercise-hypertension-prevention-treatment
